Penile Cancer Treatment
You can access compassionate, comprehensive care for penile cancer at the Montefiore Einstein Comprehensive Cancer Center. We believe each person is unique, and no two cancers are alike. For each person we serve, our cancer team develops an individualized treatment plan designed to achieve the best possible outcome.
As one of the first NCI-designated cancer centers, for more than 50 years, we've been a leader in the research, diagnosis and treatment of over 200 types of cancer.
Our penile cancer treatments are at the forefront of new and innovative methods. You can expect compassionate, personalized care that meets the highest standards for quality and safety. Our goal is to eliminate the cancer, normalize urinary function, and restore sexual function. Our patient recovery program supports these goals while providing access to nurse-led support groups.
You also benefit from our ongoing research into new, innovative treatments, some of which can be included in your care before they’re widely available if you choose to participate in one of our leading-edge cancer clinical trials. And our team is committed to whole person care and offers patients a full choice of support services and palliative care programs to meet the complex medical, emotional and spiritual needs of patients and their families.
When you need penile cancer care, turn to our providers who are passionate about ending cancer and addressing your whole health needs.

Video could not be played
Cancer Clinical Trials
- Blood & Bone Marrow Cancers
- Brain, Spine & Central Nervous System Cancers
- Breast Cancer
- Childhood Cancers
- Endocrine System Cancers
- Gastrointestinal (GI) Cancers
- Genitourinary (GU) & Urologic Cancers
- Gynecologic Cancers
- Head & Neck Cancers
- Kaposi Sarcoma & AIDS-Related Cancers
- Lung & Chest Cancers
- Prostate Cancer
- Sarcomas
- Skin Cancer
As an NCI-designated comprehensive cancer center, Montefiore Einstein Comprehensive Cancer Center supports the mission and guidelines of the National Cancer Institute (NCI). The following information about types of cancer, prevention and treatments is provided by the NCI.
Penile Cancer Treatment (PDQ®)–Patient Version
General Information About Penile Cancer
Key Points
- Penile cancer is a type of cancer that forms in the tissues of the penis.
- Human papillomavirus infection may increase the risk of developing penile cancer.
- Signs of penile cancer include sores, discharge, and bleeding.
- Tests that examine the penis are used to diagnose penile cancer.
- After penile cancer has been diagnosed, tests are done to find out if cancer cells have spread within the penis or to other parts of the body.
- Some people decide to get a second opinion.
- Certain factors affect prognosis (chance of recovery) and treatment options.
Penile cancer is a type of cancer that forms in the tissues of the penis.
The penis is a rod-shaped male reproductive organ that passes sperm and urine from the body. It contains two types of erectile tissue (spongy tissue with blood vessels that fill with blood to make an erection):
- Corpora cavernosa are the two columns of erectile tissue that form most of the penis.
- Corpus spongiosum is the single column of erectile tissue that forms a small portion of the penis. The corpus spongiosum surrounds the urethra (the tube through which urine and sperm pass from the body).
The erectile tissue is wrapped in connective tissue and covered with skin. The glans (head of the penis) is covered with loose skin called the foreskin.
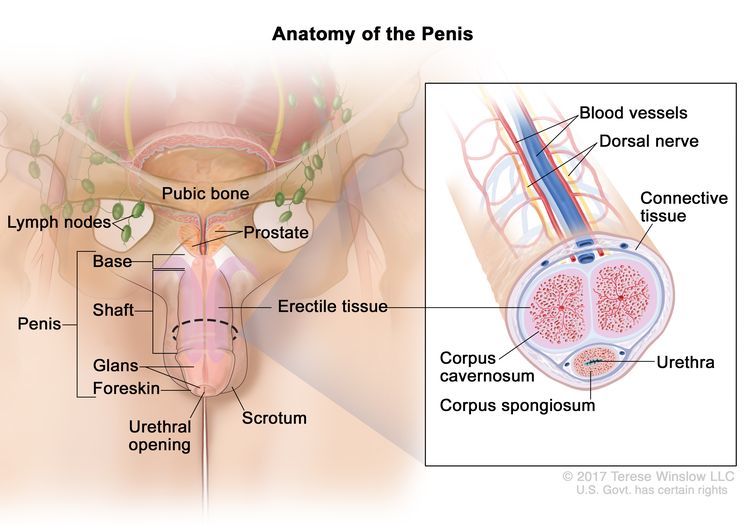
Anatomy of the penis. The parts of the penis are the base, shaft, glans, and foreskin. The tissues that make up the penis include the dorsal nerve, blood vessels, connective tissue, and erectile tissue (corpus cavernosum and corpus spongiosum). The urethra passes from the bladder to the tip of the penis.
Human papillomavirus infection may increase the risk of developing penile cancer.
Penile cancer is caused by certain changes to the penile cells function, especially how they grow and divide into new cells. There are many risk factors for penile cancer, but many do not directly cause cancer. Instead, they increase the chance of DNA damage in cells that may lead to penile cancer. To learn more about how cancer develops, see What Is Cancer?
A risk factor is anything that increases the chance of getting a disease. Some risk factors for penile cancer, such as tobacco use, can be changed. However, risk factors also include things you cannot change, like getting older and your health history. Learning about risk factors for penile cancer can help you make changes that might lower your risk of getting it.
Risk factors for penile cancer include:
- being uncircumcised. Circumcision may help prevent infection with the human papillomavirus (HPV). A circumcision is an operation in which the doctor removes part or all of the foreskin from the penis. Many boys are circumcised shortly after birth. Men who were not circumcised at birth may have a higher risk of developing penile cancer. Learn more about HPV and Cancer.
- being 60 years or older.
- having phimosis (a condition in which the foreskin of the penis cannot be pulled back over the glans).
- having poor personal hygiene.
- having many sexual partners.
- using tobacco products. Learn more about Tobacco (includes help with quitting).
Having one or more of these risk factors does not mean that you will get penile cancer. Many people with risk factors never develop penile cancer, while others with no known risk factors do. Talk with your doctor if you think you may be at risk.
Signs of penile cancer include sores, discharge, and bleeding.
These and other signs may be caused by penile cancer or by other conditions. Check with your doctor if you have:
- redness, irritation, or a sore on the penis
- a lump on the penis
Tests that examine the penis are used to diagnose penile cancer.
In addition to asking about your personal and family health history and doing a physical exam, your doctor may perform the following tests and procedures:
- Physical exam of the penis is an exam in which the doctor checks the penis for signs of disease, such as lumps or anything else that seems unusual.
- Biopsy is the removal of cells or tissues so they can be viewed under a microscope by a pathologist to check for signs of cancer. The tissue sample is removed during one of the following procedures:
- Incisional biopsy is the removal of part of a lump or a sample of tissue that doesn't look normal.
- Excisional biopsy is the removal of an entire lump or area of tissue that doesn’t look normal.
After penile cancer has been diagnosed, tests are done to find out if cancer cells have spread within the penis or to other parts of the body.
The process used to find out if cancer has spread within the penis or to other parts of the body is called staging. The information gathered from the staging process determines the stage of the disease. It is important to know the stage in order to plan treatment.
The following tests and procedures may be used in the staging process:
- CT scan (CAT scan) uses a computer linked to an x-ray machine to make a series of detailed pictures of areas inside the body, such as the pelvis. The pictures are taken from different angles and are used to create 3-D views of tissues and organs. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography.
- PET scan (positron emission tomography scan) uses a small amount of radioactive sugar (also called radioactive glucose) that is injected into a vein. The PET scanner rotates around the body and makes a picture of where the sugar is being used in the body. Cancer cells show up brighter in the picture because they are more active and take up more sugar than normal cells do. When this procedure is done at the same time as a CT scan, it is called a PET/CT scan.
- MRI (magnetic resonance imaging) uses a magnet, radio waves, and a computer to make a series of detailed pictures of areas inside the body. A substance called gadolinium is injected into a vein. The gadolinium collects around the cancer cells so they show up brighter in the picture. This procedure is also called nuclear magnetic resonance imaging (NMRI).
- Ultrasound exam uses high-energy sound waves (ultrasound), which bounce off internal tissues or organs and make echoes. The echoes form a picture of body tissues called a sonogram.
- Chest x-ray is a type of radiation that can go through the body and make pictures of the organs and bones inside the chest.
- Sentinel lymph node biopsy is the removal of the sentinel lymph node during surgery. The sentinel lymph node is the first lymph node in a group of lymph nodes to receive lymphatic drainage from the primary tumor. It is the first lymph node the cancer is likely to spread to from the primary tumor. A radioactive substance and/or blue dye is injected near the tumor. The substance or dye flows through the lymph ducts to the lymph nodes. The first lymph node to receive the substance or dye is removed. A pathologist views the tissue under a microscope to look for cancer cells. If cancer cells are not found, it may not be necessary to remove more lymph nodes. Sometimes, a sentinel lymph node is found in more than one group of nodes.
- Lymph node dissection is a procedure to remove one or more lymph nodes in the groin during surgery. A sample of tissue is checked under a microscope for signs of cancer. This procedure is also called a lymphadenectomy.
Some people decide to get a second opinion.
You may want to get a second opinion to confirm your penile cancer diagnosis and treatment plan. If you seek a second opinion, you will need to get medical test results and reports from the first doctor to share with the second doctor. The second doctor will review the pathology report, slides, and scans. They may agree with the first doctor, suggest changes or another treatment approach, or provide more information about your cancer.
Learn more about choosing a doctor and getting a second opinion at Finding Cancer Care. You can contact NCI’s Cancer Information Service via chat, email, or phone (both in English and Spanish) for help finding a doctor, hospital, or getting a second opinion. For questions you might want to ask at your appointments, visit Questions to Ask Your Doctor About Cancer.
Certain factors affect prognosis (chance of recovery) and treatment options.
The prognosis and treatment options depend on:
- the stage of the cancer
- the location and size of the tumor
- whether the cancer has just been diagnosed or has recurred (come back)
Stages of Penile Cancer
Key Points
- The following stages are used for penile cancer:
- Stage 0 (carcinoma in situ)
- Stage I (also called stage 1) penile cancer
- Stage II (also called stage 2) penile cancer
- Stage III (also called stage 3) penile cancer
- Stage IV (also called stage 4) penile cancer
- Penile cancer can recur (come back) after it has been treated.
Cancer stage describes the extent of cancer in the body, such as the size of the tumor, whether it has spread, and how far it has spread from where it first formed. It is important to know the stage of the penile cancer to plan the best treatment.
There are several staging systems for cancer that describe the extent of the cancer. Penile cancer staging usually uses the TNM staging system. The cancer may be described by this staging system in your pathology report. Based on the TNM results, a stage (I, II, III, or IV, also written as 1, 2, 3, or 4) is assigned to your cancer. When talking to you about your diagnosis, your doctor may describe the cancer as one of these stages.
Learn about tests to stage penile cancer. Learn more about Cancer Staging.
The following stages are used for penile cancer:
Stage 0 (carcinoma in situ)
Stage 0 is divided into stages 0is and 0a.
- In stage 0is, abnormal cells are found on the surface of the skin of the penis. These abnormal cells form growths that may become cancer and spread into nearby normal tissue. Stage 0is is also called carcinoma in situ or penile intraepithelial neoplasia.
- In stage 0a, squamous cell cancer that does not spread is found on the surface of the skin of the penis or on the underneath surface of the foreskin of the penis. Stage 0a is also called noninvasive localized squamous cell carcinoma.
Stage I (also called stage 1) penile cancer
In stage I, cancer has formed and spread to tissue just under the skin of the penis. Cancer has not spread to lymph vessels, blood vessels, or nerves. The cancer cells look more like normal cells under a microscope.
Stage II (also called stage 2) penile cancer
Stage II is divided into stages IIA and IIB.
In stage IIA, cancer has spread:
- to tissue just under the skin of the penis. Cancer has spread to lymph vessels, blood vessels, and/or nerves; or
- to tissue just under the skin of the penis. Under a microscope, the cancer cells look very abnormal or the cells are sarcomatoid; or
- into the corpus spongiosum (spongy erectile tissue in the shaft and glans that fills with blood to make an erection).
In stage IIB, cancer has spread:
- through the layer of connective tissue that surrounds the corpus cavernosum and into the corpus cavernosum (spongy erectile tissue that runs along the shaft of the penis).
Stage III (also called stage 3) penile cancer
Stage III is divided into stages IIIA and stage IIIB. Cancer is found in the penis.
- In stage IIIA, cancer has spread to 1 or 2 lymph nodes on one side of the groin.
- In stage IIIB, cancer has spread to 3 or more lymph nodes on one side of the groin or to lymph nodes on both sides of the groin.
Stage IV (also called stage 4) penile cancer
In stage IV, cancer has spread:
- to tissues near the penis, such as the scrotum, prostate, or pubic bone, and may have spread to lymph nodes in the groin or pelvis; or
- to one or more lymph nodes in the pelvis, or cancer has spread through the outer covering of the lymph nodes to nearby tissue; or
- to lymph nodes outside the pelvis or to other parts of the body, such as the lung, liver, or bone.
Stage IV penile cancer is also called metastatic penile cancer. Metastatic cancer happens when cancer cells travel through the lymphatic system or blood and form tumors in other parts of the body. The metastatic tumor is the same type of cancer as the primary tumor. For example, if penile cancer spreads to the liver, the cancer cells in the liver are actually penile cancer cells. The disease is called metastatic penile cancer, not liver cancer. Learn more in Metastatic Cancer: When Cancer Spreads.
Penile cancer can recur (come back) after it has been treated.
Recurrent penile cancer is cancer that has come back after it has been treated. If penile cancer comes back, it may come back in the penis or in other parts of the body, such as the liver or lungs. Tests will be done to help determine where the cancer has returned. The type of treatment for recurrent penile cancer will depend on where it has come back.
Learn more in Recurrent Cancer: When Cancer Comes Back.
Treatment Option Overview
Key Points
- There are different types of treatment for people with penile cancer.
- The following types of treatment are used:
- Surgery
- Radiation therapy
- Chemotherapy
- Immunotherapy
- New types of treatment are being tested in clinical trials.
- Treatment for penile cancer may cause side effects.
- Follow-up care may be needed.
There are different types of treatment for people with penile cancer.
Different types of treatments are available for penile cancer. You and your cancer care team will work together to decide your treatment plan, which may include more than one type of treatment. Many factors will be considered, such as the stage of the cancer, your overall health, and your preferences. Your plan will include information about your cancer, the goals of treatment, your treatment options and the possible side effects, and the expected length of treatment.
Talking with your cancer care team before treatment begins about what to expect will be helpful. You’ll want to learn what you need to do before treatment begins, how you’ll feel while going through it, and what kind of help you will need. To learn more, visit Questions to Ask Your Doctor About Treatment.
The following types of treatment are used:
Surgery
Surgery is the most common treatment for all stages of penile cancer. A doctor may remove the cancer using one of the following operations:
- Mohs microsurgery: A procedure in which the tumor is cut from the skin in thin layers. During the surgery, the edges of the tumor and each layer of tumor removed are viewed through a microscope to check for cancer cells. Layers continue to be removed until no more cancer cells are seen. This type of surgery removes as little normal tissue as possible and is often used to remove cancer on the skin. It is also called Mohs surgery.
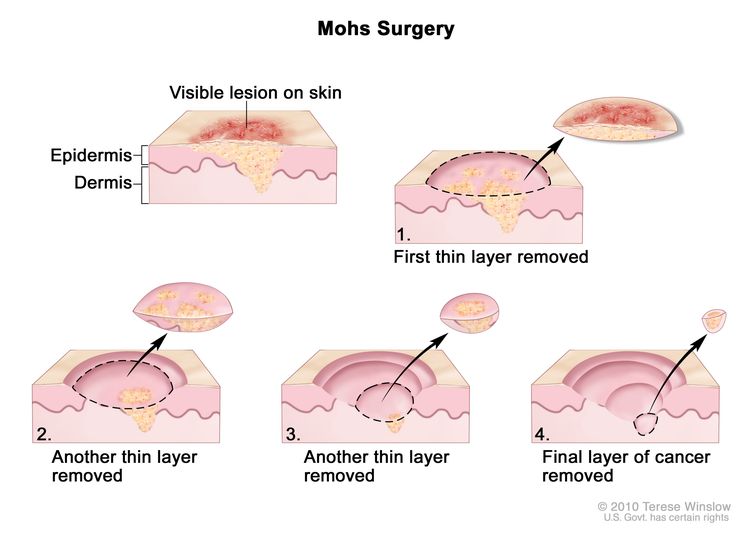
Mohs surgery. A surgical procedure to remove a visible lesion on the skin in several steps. First, a thin layer of cancerous tissue is removed. Then, a second thin layer of tissue is removed and viewed under a microscope to check for cancer cells. More layers are removed one at a time until the tissue viewed under a microscope shows no remaining cancer. This type of surgery is used to remove as little normal tissue as possible.
- Laser surgery: A surgical procedure that uses a laser beam (a narrow beam of intense light) as a knife to make bloodless cuts in tissue or to remove a surface lesion such as a tumor. Learn more about Lasers to Treat Cancer.
- Cryosurgery: A treatment that uses an instrument to freeze and destroy abnormal tissue. This type of treatment is also called cryotherapy. Learn more about Cryosurgery to Treat Cancer.
- Circumcision: Surgery to remove part or all of the foreskin of the penis.
- Wide local excision: Surgery to remove only the cancer and some normal tissue around it.
- Amputation of the penis: Surgery to remove part or all of the penis. If part of the penis is removed, it is a partial penectomy. If all of the penis is removed, it is a total penectomy.
Lymph nodes in the groin may be taken out during surgery.
After the doctor removes all the cancer that can be seen at the time of the surgery, some patients may be given chemotherapy or radiation therapy after surgery to kill any cancer cells that are left. Treatment given after the surgery, to lower the risk that the cancer will come back, is called adjuvant therapy.
Radiation therapy
Radiation therapy is a cancer treatment that uses high-energy x-rays or other types of radiation to kill cancer cells or keep them from growing. There are two types of radiation therapy used to treat penile cancer:
- External radiation therapy uses a machine outside the body to send radiation toward the area of the body with cancer.
- Internal radiation therapy uses a radioactive substance sealed in needles, seeds, wires, or catheters that are placed directly into or near the cancer.
Learn more about Radiation Therapy to Treat Cancer and Radiation Therapy Side Effects.
Chemotherapy
Chemotherapy (also called chemo) uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing.
Topical chemotherapy is placed directly onto the skin, where it mainly affects cancer cells in those areas. Topical chemotherapy, such as fluorouracil may be used to treat stage 0 penile cancer.
Systemic chemotherapy is when chemotherapy drugs are taken by mouth or injected into a vein or muscle. When given this way, the drugs enter the bloodstream and can reach cancer cells throughout the body. Systemic chemotherapy may be used if the cancer is too large to be removed by surgery or has spread to the lymph nodes or other parts of the body.
Learn more about how chemotherapy works, how it is given, common side effects, and more at Chemotherapy to Treat Cancer and Chemotherapy and You: Support for People With Cancer.
Immunotherapy
Immunotherapy helps a person’s immune system fight cancer.
Topical imiquimod is an immunotherapy drug used to treat penile cancer.
Learn more about Immunotherapy to Treat Cancer.
New types of treatment are being tested in clinical trials.
For some people, joining a clinical trial may be an option. There are different types of clinical trials for people with cancer. For example, a treatment trial tests new treatments or new ways of using current treatments. Supportive care and palliative care trials look at ways to improve quality of life, especially for those who have side effects from cancer and its treatment.
You can use the clinical trial search to find NCI-supported cancer clinical trials accepting participants. The search allows you to filter trials based on the type of cancer, your age, and where the trials are being done. Clinical trials supported by other organizations can be found on the ClinicalTrials.gov website.
Learn more about clinical trials, including how to find and join one, at Clinical Trials Information for Patients and Caregivers.
Treatment for penile cancer may cause side effects.
For information about side effects caused by treatment for cancer, visit our Side Effects page.
Follow-up care may be needed.
As you go through treatment, you will have follow-up tests or check-ups. Some tests that were done to diagnose or stage the cancer may be repeated to see how well the treatment is working. Decisions about whether to continue, change, or stop treatment may be based on the results of these tests.
Some of the tests will continue to be done from time to time after treatment has ended. The results of these tests can show if your condition has changed or if the cancer has recurred (come back).
Treatment of Stage 0
Treatment of stage 0 may include:
- Mohs microsurgery
- topical chemotherapy
- topical immunotherapy with imiquimod
- laser surgery
- cryosurgery
Learn more about these treatments in the Treatment Option Overview.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Stage I Penile Cancer
If the cancer is only in the foreskin, wide local excision and circumcision may be the only treatment needed.
Treatment of stage I penile cancer may also include:
- surgery (partial or total penectomy with or without removal of lymph nodes in the groin)
- external or internal radiation therapy
- Mohs microsurgery
Learn more about these treatments in the Treatment Option Overview.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Stage II Penile Cancer
Treatment of stage II penile cancer may include:
- surgery (partial or total penectomy, with or without removal of lymph nodes in the groin)
- external or internal radiation therapy followed by surgery
Learn more about these treatments in the Treatment Option Overview.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Stage III Penile Cancer
Treatment of stage III penile cancer may include:
- surgery (penectomy and removal of lymph nodes in the groin) with or without radiation therapy
- radiation therapy
Learn more about these treatments in the Treatment Option Overview.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Stage IV Penile Cancer
Treatment of stage IV penile cancer is usually palliative (to relieve symptoms and improve the quality of life). Treatment may include:
- surgery (wide local excision and removal of lymph nodes in the groin)
- radiation therapy
Learn more about these treatments in the Treatment Option Overview.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Recurrent Penile Cancer
Treatment of recurrent penile cancer may include:
- surgery (penectomy)
- radiation therapy
Learn more about these treatments in the Treatment Option Overview.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
To Learn More About Penile Cancer
For more information from the National Cancer Institute about penile cancer, visit:
For general cancer information and other resources from the National Cancer Institute, visit:
About This PDQ Summary
About PDQ
Physician Data Query (PDQ) is the National Cancer Institute's (NCI's) comprehensive cancer information database. The PDQ database contains summaries of the latest published information on cancer prevention, detection, genetics, treatment, supportive care, and complementary and alternative medicine. Most summaries come in two versions. The health professional versions have detailed information written in technical language. The patient versions are written in easy-to-understand, nontechnical language. Both versions have cancer information that is accurate and up to date and most versions are also available in Spanish.
PDQ is a service of the NCI. The NCI is part of the National Institutes of Health (NIH). NIH is the federal government’s center of biomedical research. The PDQ summaries are based on an independent review of the medical literature. They are not policy statements of the NCI or the NIH.
Purpose of This Summary
This PDQ cancer information summary has current information about the treatment of penile cancer. It is meant to inform and help patients, families, and caregivers. It does not give formal guidelines or recommendations for making decisions about health care.
Reviewers and Updates
Editorial Boards write the PDQ cancer information summaries and keep them up to date. These Boards are made up of experts in cancer treatment and other specialties related to cancer. The summaries are reviewed regularly and changes are made when there is new information. The date on each summary ("Updated") is the date of the most recent change.
The information in this patient summary was taken from the health professional version, which is reviewed regularly and updated as needed, by the PDQ Adult Treatment Editorial Board.
Clinical Trial Information
A clinical trial is a study to answer a scientific question, such as whether one treatment is better than another. Trials are based on past studies and what has been learned in the laboratory. Each trial answers certain scientific questions in order to find new and better ways to help cancer patients. During treatment clinical trials, information is collected about the effects of a new treatment and how well it works. If a clinical trial shows that a new treatment is better than one currently being used, the new treatment may become "standard." Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
Clinical trials can be found online at NCI's website. For more information, call the Cancer Information Service (CIS), NCI's contact center, at 1-800-4-CANCER (1-800-422-6237).
Permission to Use This Summary
PDQ is a registered trademark. The content of PDQ documents can be used freely as text. It cannot be identified as an NCI PDQ cancer information summary unless the whole summary is shown and it is updated regularly. However, a user would be allowed to write a sentence such as “NCI’s PDQ cancer information summary about breast cancer prevention states the risks in the following way: [include excerpt from the summary].”
The best way to cite this PDQ summary is:
PDQ® Adult Treatment Editorial Board. PDQ Penile Cancer Treatment. Bethesda, MD: National Cancer Institute. Updated <MM/DD/YYYY>. Available at: https://www.cancer.gov/types/penile/patient/penile-treatment-pdq. Accessed <MM/DD/YYYY>. [PMID: 26389255]
Images in this summary are used with permission of the author(s), artist, and/or publisher for use in the PDQ summaries only. If you want to use an image from a PDQ summary and you are not using the whole summary, you must get permission from the owner. It cannot be given by the National Cancer Institute. Information about using the images in this summary, along with many other images related to cancer can be found in Visuals Online. Visuals Online is a collection of more than 3,000 scientific images.
Disclaimer
The information in these summaries should not be used to make decisions about insurance reimbursement. More information on insurance coverage is available on Cancer.gov on the Managing Cancer Care page.
Contact Us
More information about contacting us or receiving help with the Cancer.gov website can be found on our Contact Us for Help page. Questions can also be submitted to Cancer.gov through the website’s E-mail Us.
Updated:
Source URL: https://www.cancer.gov/node/5940/syndication
Source Agency: National Cancer Institute (NCI)
Captured Date: 2013-09-14 09:03:13.0